
More Allergy, Asthma & Infectious Disease Articles
Is Eczema an Autoimmune Condition? Understanding the Connection
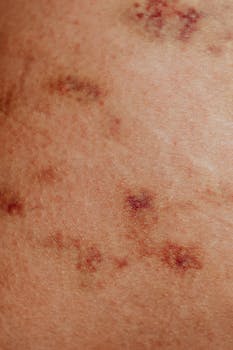
Eczema is a common skin condition characterized by inflammation and an itchy rash. Many people wonder, is eczema autoimmune? This question arises because eczema often occurs alongside other immune-related conditions.
Is Eczema Autoimmune?
Eczema, also known as atopic dermatitis, is primarily considered an inflammatory skin condition rather than a classic autoimmune disease. In autoimmune diseases, the body’s immune system mistakenly attacks its own tissues. With eczema, the issue lies more with the skin’s inability to retain moisture and protect itself against irritants, allergens, and bacteria. However, the immune system does play a significant role in eczema. The condition is associated with an overactive immune response to environmental triggers, leading to the symptoms of red, itchy, and inflamed skin.
Understanding Eczema and the Immune System
Eczema involves a complex interaction between genetic and environmental factors. It’s linked to variations in the genes that control proteins responsible for maintaining the skin’s barrier. When these proteins are deficient or non-functional, the skin barrier is weakened, increasing susceptibility to irritants and infections, leading to inflammation.
The immune response in eczema is thought to be hyperactive, similar to that seen in many autoimmune diseases. Nevertheless, since eczema doesn’t involve the direct attack of self-tissues by the immune system, it is not classified strictly as autoimmune. The distinction between eczema and autoimmune disorders can be subtle but is crucial for understanding the nature of the condition and its management.
Eczema’s Relation to Other Conditions
People with eczema often have other conditions like asthma or allergic rhinitis, collectively referred to as the atopic triad. This interrelation suggests a common underlying issue within immune system regulation.Functional medicine approaches may help identify and manage these interconnected concerns by addressing the precursor elements that may trigger these conditions.
Managing Eczema Symptoms
Management of eczema involves both skincare and addressing immune responses. Moisturizing and protecting the skin barrier are foundational steps. Topical treatments, such as corticosteroids and calcineurin inhibitors, are often employed to reduce inflammation and itching. Moreover, new biologic medications that target specific pathways in the immune system show promise for severe cases. Lifestyle changes, like stress management and identifying dietary triggers, can also play a critical role.
While eczema itself is not autoimmune, it is essential to manage the immune system’s hyperactivity. Approaches that combine both traditional and integrative therapies are often most beneficial for individuals seeking comprehensive management of their symptoms.
Future Research and Considerations
Ongoing research continues to explore the exact mechanisms of eczema. Understanding these could lead to more targeted therapies that address both the skin’s barrier function and immune dysregulation. Some studies suggest a potential role for probiotics and omega-3 fatty acids in modulating immune response and supporting skin health, although these interventions require further evidence to confirm their efficacy.
Researchers are intrigued by the overlap between eczema, other atopic conditions, and autoimmune diseases as they consider the future of treatment and prevention strategies. This interest underlines the importance of studying eczema as part of a broader pattern of immune-related conditions.
Conclusion: Is Eczema Autoimmune?
In summary, while eczema involves an overactive immune system, it is not classified as an autoimmune disease. Advances in understanding and treatment continue to improve quality of life for individuals with eczema. If you’re interested in learning more about health topics, you can visit reliable resources such as the Health page on Wikipedia.
Takeaways
- Eczema primarily involves skin inflammation, not autoimmunity.
- The immune system plays a significant role in exacerbating eczema symptoms.
- Management requires restoring the skin barrier and regulating immune response.
- Ongoing research focuses on new treatments and understanding immune interactions.
- Professional consultation is crucial for personalized eczema management.
FAQ
What triggers eczema flare-ups?
Common triggers include allergens, irritants, stress, and changes in weather. Identifying personal triggers can help manage flare-ups effectively.
Can dietary changes help manage eczema?
Some individuals find relief by avoiding specific food triggers, though dietary changes should be discussed with a healthcare provider for personalized advice.
How is eczema diagnosed?
Diagnosis is typically based on the physical examination of the skin and medical history. Sometimes, additional tests may be needed to rule out other conditions.
Are there new treatments for eczema?
Yes, biologic therapies and targeted treatments continue to evolve, offering new options for individuals with severe eczema.
How does functional medicine approach eczema?
Functional medicine focuses on identifying and addressing underlying triggers and imbalances, offering a holistic approach to managing eczema.
Other Articles You May Find of Interest...
- What Does a Normal FEV1 Indicate About Your Lung Health?
- Arterial Blood Gas Explained: Importance and Interpretation for Your Health
- Decoding the SFA Medical Abbreviation for Better Health Awareness
- Is Your Varicella Titer Protecting You from Chickenpox?
- Protecting Your Health: The Impact of Invasive Pneumococcal Disease
- Unlocking the Secrets of Milliliters and Milligrams for Better Health
- Managing Parapneumonic Effusion: Essential Insights for Better Health














