
Your Health Magazine
4201 Northview Drive
Suite #102
Bowie, MD 20716
301-805-6805

More Legal and Health Articles
What Goes Wrong With Fetal Monitoring in Florida and Why It Matters
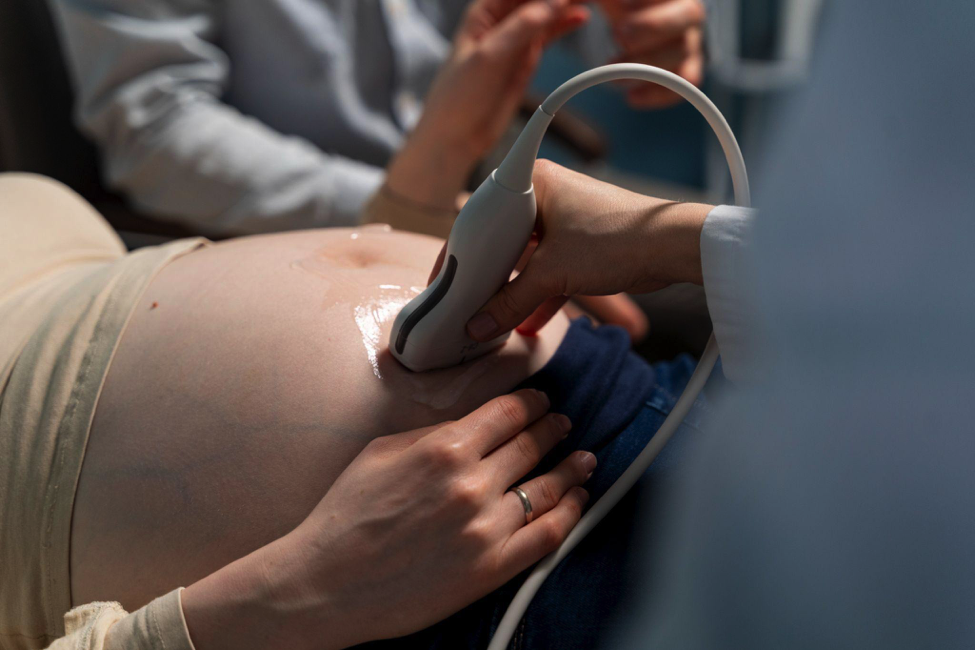
Fetal monitoring during labor is meant to show whether a baby is tolerating contractions or showing signs of distress. When the tracing is misread, lost, or ignored, the result can be a delayed response to oxygen deprivation, infection, cord compression, or excessive uterine activity. In Florida, those events can raise both medical and legal questions because birth injury claims often move through the state’s medical negligence rules, and a narrow set of severe neurological injuries may fall under a separate no-fault system.
What Fetal Monitoring Is Meant To Show
During labor, clinicians use continuous electronic monitoring to track the baby’s heart rate alongside contractions. In cases involving fetal monitoring mistakes in Florida, the first questions usually focus on whether the tracing was captured clearly and whether the staff interpreted it correctly. A weak signal, gaps in the record, or a delay in reviewing the strip can affect how clinicians respond during labor. The goal is to identify whether the baby is tolerating labor and to trigger a prompt response when the pattern changes.
Current obstetric practice places fetal heart tracings into three categories. Category I is generally reassuring, Category II calls for closer assessment and corrective action, and Category III raises concern for abnormal acid-base status when it does not improve quickly. This framework helps labor teams decide whether continued observation, bedside intervention, or expedited delivery may be appropriate.
Common Sources Of Error
Some mistakes happen before anyone even interprets the strip. The monitor may pick up the mother’s pulse instead of the baby’s, the signal may drop out during movement, or the tracing may be poorly documented, leaving gaps at the very time the labor pattern mattered most.
Other mistakes involve response, not equipment. Recurrent late decelerations, prolonged bradycardia, or contractions coming too close together can require prompt measures such as repositioning, stopping uterine-stimulating medication, giving fluids, or moving toward delivery if the tracing does not recover.
Why Delays Can Change The Outcome
Timing matters because fetal oxygen problems can worsen over minutes, not days. A strip that looks indeterminate at first can become far more concerning when decreased variability, repeated decelerations, or a sustained slow heart rate continue without improvement.
That is why the written record matters almost as much as the strip itself. Notes about when the pattern changed, who was notified, what interventions were tried, and when delivery occurred often shape later review of whether the response matched the situation.
How Florida Law Frames These Disputes
In Florida, a claim that hospital staff or clinicians mishandled labor monitoring is usually treated as a medical negligence case. Before filing suit, a claimant must complete a presuit investigation and send notice of intent to each prospective defendant, and relevant medical records must be produced within 10 business days at a reasonable charge in most cases.
Deadlines also matter. Florida generally gives two years from the incident, or from when the injury was discovered or should have been discovered with due diligence, with a four-year outside limit in most cases, although claims on behalf of a minor may be brought on or before the child’s eighth birthday and fraud-based concealment can extend the period up to seven years, still subject to the minor exception. When fetal monitoring decisions are questioned after delivery, the issue can move from a medical review to a legal one.
When A Birth Injury Claim May Not Stay In Court
Florida also has the Birth-Related Neurological Injury Compensation Plan, often called NICA. For qualifying birth-related neurological injuries involving a participating physician, that administrative remedy can replace an ordinary negligence suit against those directly involved in labor, delivery, or immediate postdelivery resuscitation, unless the statutory bad-faith or willful-misconduct exception applies.
That distinction matters because a family may be dealing with two separate questions at once: what the fetal monitor showed, and whether the claim belongs in court or in the NICA system. Florida law also requires hospitals with participating physicians, and the participating physicians themselves, to give obstetrical patients notice of that limited no-fault alternative, except in emergencies or when notice is not practicable.
Why This Issue Reaches Beyond The Delivery Room
Fetal monitoring disputes rarely turn on a single alarming moment. They usually turn on a sequence: what the strip showed, whether the team recognized the pattern, how quickly they acted, and which Florida legal pathway applies once the records are reviewed. Medical records, monitoring strips, and hospital documentation often become central evidence when those events are examined later.
Other Articles You May Find of Interest...
- What Goes Wrong With Fetal Monitoring in Florida and Why It Matters
- Who Qualifies for Workers’ Comp Death Benefits in Orlando?
- Objective Analysis: Staying Neutral as a Medical Expert Witness
- The Legality of Peptides: What You Need to Know
- New York’s No-Fault Insurance Law: How It Works, What It Covers, and the Threshold That Determines Whether You Can Sue
- Don’t Walk Away Empty-Handed: The Truth About Shared Fault in AZ Car Wrecks
- How To Approach End-of-Life Decisions With Clarity and Care














