
Your Health Magazine
4201 Northview Drive
Suite #102
Bowie, MD 20716
301-805-6805

More Dental Health Articles
Benefits of Dental Implants and How They Improve Your Smile
Nearly 70% of American adults have lost at least one permanent tooth by age 44, according to the American College of Prosthodontists—and that number is rising as our population ages. What’s more concerning is that traditional tooth replacement options often create a cascade of additional oral health problems, from bone loss to adjacent tooth damage. The dental implant industry has experienced explosive growth over the past decade, with success rates now exceeding 95% in healthy patients, fundamentally changing how we think about tooth replacement.
The stakes couldn’t be higher. Beyond the obvious aesthetic concerns, missing teeth affect everything from nutrition and speech to self-confidence and social interaction. Yet many people still rely on outdated solutions like removable dentures or bridges that can actually accelerate oral health decline. Modern dental implants offer something fundamentally different: they’re the only tooth replacement option that preserves jawbone integrity while restoring full function, making it important to explore the available dental implant options in New Brunswick for personalized care.
Here’s what the latest research and clinical evidence reveal about why dental implants have become the gold standard for tooth replacement, and how they deliver benefits that extend far beyond just filling gaps in your smile.
What Are Dental Implants and How Do They Work?
Think of dental implants as artificial tooth roots that your body actually accepts and integrates with. Unlike dentures that sit on top of your gums or bridges that rely on adjacent teeth for support, implants are surgically placed directly into your jawbone, where they fuse with the bone tissue through a process called osseointegration.
This integration process is what makes implants so remarkable. The implant itself—typically made from biocompatible titanium—actually stimulates your jawbone the same way natural tooth roots do. When you chew or bite down, the force travels through the implant directly into the bone, maintaining healthy bone density and preventing the facial collapse that often occurs with traditional dentures.
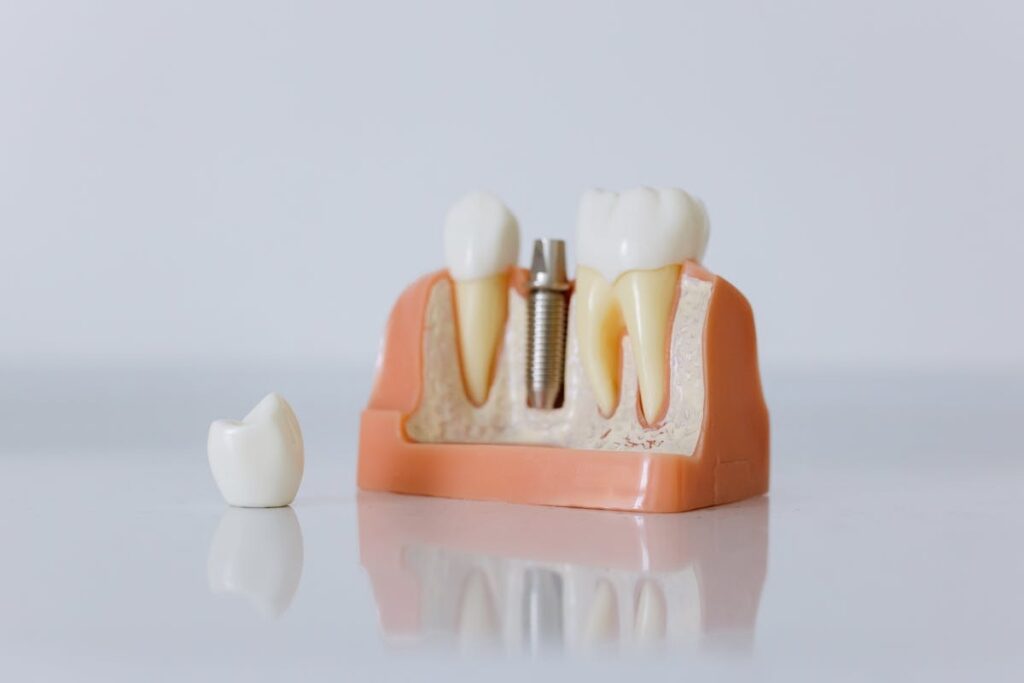
The complete implant system consists of three components: the titanium post that goes into the bone, an abutment that connects to the post, and the crown that looks and functions like your natural tooth. This three-part design allows for customization and repair if needed, while the titanium post provides the structural foundation that can last decades.
What sets this apart from other tooth replacement options is the biological integration. Your bone tissue doesn’t just accept the implant—it actively grows around it, creating a permanent, stable foundation. This is why patients often report that implants feel more natural than their original teeth, especially if those teeth were compromised by decay or damage before extraction.
What Happens During Dental Implant Surgery?
Step-By-Step Dental Implant Procedure Explained
The implant placement process typically unfolds in carefully planned stages, though the exact timeline varies based on individual healing capacity and bone quality. During the initial surgical phase, your oral surgeon creates a precise opening in the jawbone using specialized drilling techniques that preserve surrounding bone structure. The titanium implant is then placed with exact positioning—typically within millimeters of the planned location determined through 3D imaging.
What happens next is where the real magic occurs. Over the following 3-6 months, your bone tissue begins growing around the implant surface through osseointegration. This isn’t just healing—it’s your body literally incorporating the implant as part of your skeletal structure. Modern implant surfaces are designed with microscopic textures that encourage this bone growth, creating a bond that’s actually stronger than the connection between natural teeth and bone.
Once integration is complete, the second phase involves attaching the abutment and custom crown. Advanced digital scanning now allows for precise crown fabrication that matches your bite pattern exactly. The entire process, from placement to final restoration, typically takes 4-8 months, though immediate loading protocols can sometimes reduce this timeline significantly.
Differences Between Immediate and Delayed Implant Placement
The timing of implant placement relative to tooth extraction represents one of the most significant advances in implant dentistry. Immediate placement involves inserting the implant at the same time as tooth extraction, potentially reducing treatment time by several months. However, this approach requires adequate bone volume and ideal healing conditions.
Delayed placement, the traditional approach, allows 3-4 months of healing after extraction before implant surgery. While this extends the overall timeline, it provides optimal conditions for implant success, especially in cases where bone grafting is needed or infection was present. Recent studies show comparable long-term success rates between approaches when patient selection criteria are carefully followed.
The decision between immediate and delayed placement depends on factors like bone quality, gum tissue health, and the reason for tooth loss. Immediate placement works best for healthy teeth lost due to trauma, while delayed placement is often preferred when treating teeth lost due to infection or severe periodontal disease.
What Types of Dental Implants Are Used in Treatment?
Endosteal implants, the most common type, are placed directly into the jawbone and account for over 90% of all implant procedures. These screw-shaped implants come in various diameters and lengths to accommodate different anatomical situations. The surface treatments on modern endosteal implants—including sandblasted, acid-etched surfaces—significantly improve osseointegration rates compared to earlier smooth-surface designs.
Subperiosteal implants represent a specialized solution for patients with insufficient bone height who cannot or choose not to undergo bone grafting procedures. These custom-fabricated frameworks sit on top of the bone but underneath the gum tissue, providing support for multiple teeth. While less common today due to advances in bone grafting techniques, they remain valuable for specific anatomical challenges.
Zygomatic implants offer a solution for severe upper jaw bone loss by anchoring into the cheekbone rather than the maxillary bone. These longer implants bypass areas of bone deficiency, enabling immediate function even in cases where traditional implants wouldn’t be possible without extensive grafting procedures.
The choice of implant type and material significantly impacts both short-term healing and long-term outcomes. Titanium remains the gold standard due to its biocompatibility and proven track record, though newer materials like zirconia are gaining acceptance for patients with specific aesthetic requirements or metal sensitivities. Understanding these options helps explain why implant treatment can be customized to virtually any clinical situation.
How Do Dental Implants Benefit Oral Health and Jawbone Integrity?
The most profound benefit of dental implants lies in their ability to preserve jawbone structure—something no other tooth replacement option can achieve. When you lose a tooth, the surrounding bone begins resorbing immediately, losing up to 25% of its width within the first year alone. This process accelerates over time, leading to the sunken facial appearance often associated with long-term tooth loss.
Implants interrupt this destructive cycle by providing the mechanical stimulation your bone needs to maintain density. Every time you chew, the force transmitted through the implant signals your body to maintain bone tissue in that area. Research published in the Journal of Periodontology shows that areas with implants maintain 98% of original bone volume over 10-year periods, compared to 40-60% loss in areas with missing teeth.
This bone preservation creates a ripple effect of benefits. Your remaining natural teeth maintain proper support and alignment, reducing risk of additional tooth loss. Your gums stay healthy because implants provide stable tissue support, unlike removable prosthetics that can cause chronic irritation. The facial structure remains intact, preventing the premature aging appearance that occurs when multiple teeth are lost.
Perhaps most importantly, implants can actually improve your overall oral health by making proper hygiene easier to maintain. Unlike bridges that create hard-to-clean areas underneath, or dentures that trap food particles, implants can be brushed and flossed just like natural teeth. This accessibility significantly reduces your risk of developing gum disease or decay in adjacent teeth—problems that often lead to additional tooth loss down the road.
In What Ways Do Dental Implants Enhance Function and Quality of Life?
The functional improvements with dental implants extend far beyond basic chewing ability. Studies consistently show that implant patients can generate bite forces of 200-250 pounds per square inch—comparable to natural teeth and roughly three times stronger than what’s possible with conventional dentures. This restored chewing efficiency directly impacts nutrition, allowing patients to maintain diets rich in fresh fruits, vegetables, and proteins that might otherwise be difficult to consume.
Speech clarity represents another dramatic improvement area. Missing teeth, particularly in the front of the mouth, can cause lisping, whistling, or unclear pronunciation. Ill-fitting dentures often make these problems worse by shifting during speech or requiring adhesives that affect tongue movement. Implants provide the stable foundation necessary for clear speech, with patients typically reporting improved confidence in professional and social situations within weeks of treatment completion.
The psychological benefits often prove as significant as the physical ones. Research from the International Journal of Oral and Maxillofacial Implants found that implant patients showed measurable improvements in self-esteem, social confidence, and overall quality of life scores compared to those with conventional prosthetics. The knowledge that your teeth won’t shift, slip, or require special maintenance routines provides a psychological freedom that many patients describe as “life-changing.”
Convenience factors add another layer of benefit. Implants eliminate the daily removal and cleaning routines required with dentures, the dietary restrictions necessary with bridges, and the ongoing adjustments often needed as your mouth changes over time. You simply brush, floss, and maintain regular dental checkups—the same routine you’d follow with natural teeth.
How Do Dental Implants Compare With Dentures and Bridges?
The stability difference between implants and conventional dentures becomes immediately apparent during basic activities like eating or speaking. Conventional dentures rely on suction and adhesives for retention, which can fail unpredictably and often limits food choices to softer textures. Even well-fitted dentures typically reduce chewing efficiency by 60-70% compared to natural teeth, while implant-supported restorations maintain nearly full chewing capacity.
Longevity represents perhaps the most compelling comparison point. While dentures typically require replacement every 5-7 years and frequent adjustments due to ongoing bone loss, quality dental implants can last 25-30 years or more with proper care. Bridges, though more stable than dentures, average 10-15 years before replacement is needed and require modification of healthy adjacent teeth that weakens them over time.
From an oral health perspective, implants are the only option that preserves your existing dental structure. Bridges require grinding down adjacent healthy teeth to serve as anchors, permanently weakening them and increasing future failure risk. Partial dentures often accelerate bone loss and can contribute to decay or gum disease around the clasps that hook onto remaining teeth.
The cost analysis becomes more favorable for implants when viewed over decades rather than years. While the initial investment is typically higher, the lack of ongoing adjustments, replacements, and potential complications often makes implants more economical long-term. Insurance coverage for implants continues expanding as more providers recognize their clinical superiority and cost-effectiveness over time.
What Are the Key Factors for Dental Implant Success and Longevity?
Patient selection remains the most critical factor in implant success, with certain medical conditions and lifestyle factors significantly impacting outcomes. Adequate bone volume and density provide the foundation for successful osseointegration, which is why thorough 3D imaging evaluation is essential before treatment planning. Patients with uncontrolled diabetes, heavy smokers, or those taking certain medications may experience higher failure rates and require modified treatment protocols.
The surgical technique and experience level of your implant team directly correlates with long-term success. Research consistently shows that surgeons placing more than 50 implants annually achieve success rates 5-8% higher than those with limited experience. Precise implant positioning, proper drilling protocols that avoid overheating bone tissue, and sterile technique all contribute to optimal healing and integration.
Maintenance habits play an equally important role in long-term implant health. While implants can’t develop decay, the surrounding gum tissue remains susceptible to inflammation and infection. Patients who maintain excellent oral hygiene and attend regular professional cleanings experience success rates above 95% at 10-year follow-ups, compared to 85-90% success in patients with poor maintenance habits.
The quality of the implant components themselves has improved dramatically over the past decade. Modern implant surfaces, precision-machined connections, and advanced crown materials all contribute to longevity. However, the biological factors—your body’s healing response, bone quality, and ongoing oral health—ultimately determine whether an implant will last 15 years or 40 years.
What Are the Potential Risks and How Is Recovery Managed?
Like any surgical procedure, dental implant placement carries inherent risks, though serious complications occur in fewer than 5% of cases when performed by experienced clinicians. Infection represents the most common concern, typically manifesting as persistent pain, swelling, or drainage around the implant site. Most infections respond well to antibiotic therapy when caught early, though severe cases may require implant removal and delayed replacement.
Nerve damage, while rare, can occur if implants are placed too close to major nerve pathways in the lower jaw. This risk is virtually eliminated through proper pre-surgical planning using 3D imaging and computer-guided placement techniques. When nerve irritation does occur, it’s usually temporary and resolves within a few months as healing progresses.
Implant failure typically falls into two categories: early failure due to poor healing or infection, and late failure due to bone loss around a previously successful implant. Early failures often relate to surgical technique, patient healing capacity, or post-operative complications. Late failures usually result from poor maintenance, smoking, or systemic health changes that affect bone metabolism.
Recovery management focuses on promoting optimal healing while minimizing complications. Most patients experience mild discomfort for 3-5 days that responds well to over-the-counter pain medication. Avoiding hard foods, maintaining gentle oral hygiene, and following prescribed antibiotic regimens significantly reduce infection risk. Smoking cessation during the healing period is crucial, as nicotine dramatically impairs blood supply and can double the failure rate.
What Are the Recent Advances and Future Trends in Dental Implant Technology?
Digital workflow integration has revolutionized implant planning and placement accuracy over the past five years. Computer-guided surgery now allows surgeons to plan implant positions virtually and transfer that plan precisely to the patient’s mouth using specialized surgical guides. This technology reduces surgery time, improves positioning accuracy, and often eliminates the need for traditional surgical flaps, resulting in faster healing and less post-operative discomfort.
Surface technology advances continue improving osseointegration speed and success rates. Modern implant surfaces incorporate nanotechnology, specialized coatings, and microscopic surface modifications that encourage faster bone growth and stronger integration. Some newer surfaces can achieve clinically significant integration in as little as 6-8 weeks, compared to the traditional 3-4 month healing period.
Immediate loading protocols represent another significant advancement, allowing patients to receive functional teeth on the same day as implant placement in carefully selected cases. While not appropriate for every situation, immediate loading can dramatically reduce treatment time and improve patient satisfaction when proper criteria are met.
Looking ahead, researchers are developing bioactive implant surfaces that release growth factors to accelerate healing, and exploring stem cell therapy to regenerate bone tissue around implants. Artificial intelligence is beginning to assist in treatment planning and outcome prediction, potentially improving success rates further while reducing treatment complexity. These innovations suggest that implant therapy will become even more predictable, faster, and accessible in the coming decade, cementing its position as the definitive solution for tooth replacement.
Other Articles You May Find of Interest...
- 5 Best Toothpastes for Plaque Removal: Why Your Current Toothpaste Isn’t Cutting It
- How to Choose the Right Toothpaste for Your Family’s Dental Needs
- How to Choose the Right Dentist for Your Family in Toronto
- How Dental Nutrition Supplements Support Strong Teeth And Gums
- Braces Treatment Options and Their Benefits Explained
- How Cosmetic Dentistry in Naples Transforms Smiles and Confidence
- What to Do if You’re Missing a Tooth: Solutions and Health Impacts














