
Your Health Magazine Contributor
4201 Northview Drive
Suite #102
Bowie, MD 20716
301-805-6805

More Pet Health Articles
Understanding Common Types of Pet Surgical Procedures
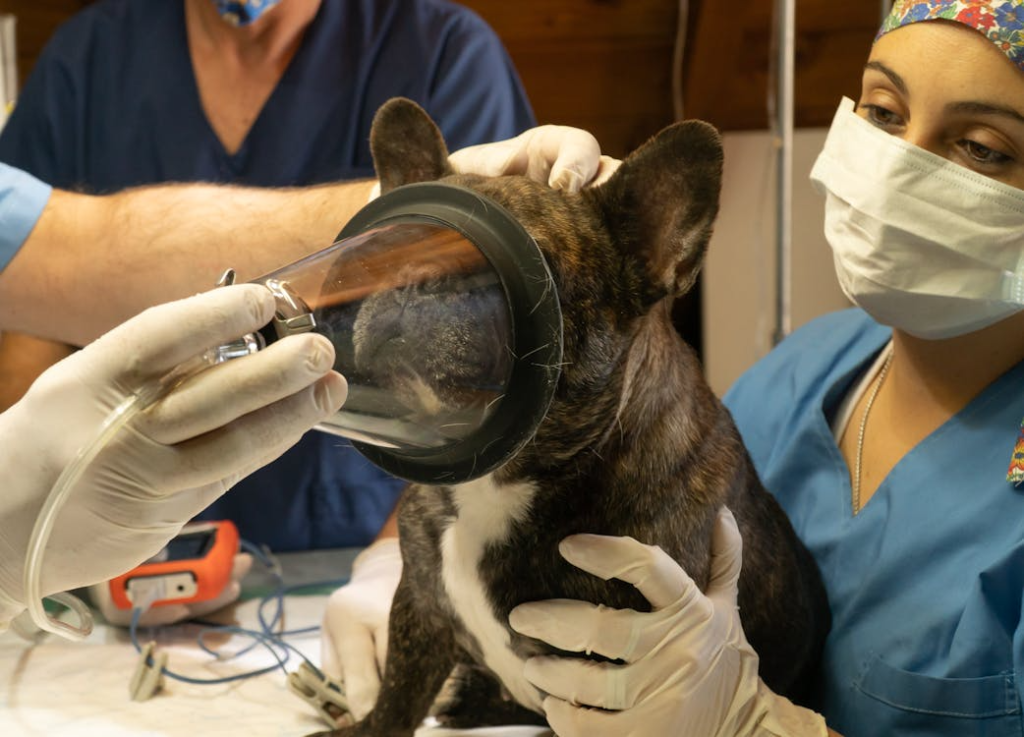
The American Veterinary Medical Association reports that over 3 million pets undergo surgery annually in the United States, with spaying and neutering accounting for roughly 60% of all procedures. Yet when emergency situations arise — from torn ligaments to intestinal blockages — many pet owners find themselves unprepared for the complexity of modern veterinary surgery. As veterinary medicine continues to advance with minimally invasive techniques and sophisticated anesthesia protocols, the gap between what owners expect and what’s actually involved in surgical care has never been wider. Understanding the landscape of pet surgeries, from routine procedures to complex interventions, helps owners make informed decisions when their companion’s health is on the line.
What Are the Most Common Types of Pet Surgeries
Veterinary surgeries fall into several distinct categories, each with different risk profiles, preparation requirements, and recovery expectations. Elective procedures — those scheduled in advance for health maintenance — represent the majority of surgical cases veterinarians perform. Emergency surgeries address immediate threats to life or limb, while orthopedic interventions focus on bones, joints, and supporting structures. Soft tissue surgeries encompass everything from tumor removals to gastrointestinal repairs.
The distinction between these categories matters more than most owners realize. Elective surgeries allow for optimal timing, thorough pre-surgical evaluation, and careful preparation. Emergency procedures, by contrast, often require rapid decision-making with limited diagnostic information. A dog with a twisted stomach (gastric dilatation-volvulus) needs immediate surgical intervention, regardless of whether the timing is ideal for anesthesia or recovery.
Consider the difference between scheduling a cat’s spay surgery versus rushing that same cat to the emergency room for a urinary blockage. The spay surgery can be planned around the pet’s health status, the owner’s schedule, and optimal staffing. The urinary blockage demands immediate action, often requiring surgery within hours to prevent kidney damage or death.
Elective Surgeries and Their Role in Pet Health
Spaying and neutering represent the foundation of elective veterinary surgery, performed on millions of pets annually to prevent reproduction and reduce disease risk. These procedures involve removing reproductive organs — ovaries and uterus in females, testicles in males — through carefully standardized surgical approaches that have evolved significantly over the past decade.
Modern spay techniques have moved away from the traditional large abdominal incision toward more precise approaches. Many veterinarians now perform ovariectomies (removing just the ovaries) rather than complete ovariohysterectomies, reducing surgical time and post-operative discomfort while achieving the same reproductive and health benefits. The timing of these surgeries has also shifted, with many practitioners recommending procedures before the first heat cycle to maximize cancer prevention benefits.
Mass removals constitute another major category of elective surgery, addressing everything from benign lipomas to suspicious skin growths. These procedures require careful surgical planning to ensure complete removal while preserving function and appearance. When veterinarians recommend removing a growth, they’re weighing factors like the mass’s growth rate, location, and potential for malignancy against the risks of surgery and anesthesia.
Dental surgeries round out the most common elective procedures, addressing periodontal disease, tooth extractions, and oral masses. These surgeries require general anesthesia to allow thorough cleaning, assessment, and treatment of dental problems that can’t be adequately addressed in awake patients.
How Surgery Techniques and Anesthesia Affect Pet Outcomes
The foundation of safe pet surgery rests on sophisticated anesthesia protocols tailored to each animal’s species, breed, age, and health status. Modern veterinary anesthesia goes far beyond simply rendering an animal unconscious — it involves carefully balanced combinations of medications that provide unconsciousness, pain relief, muscle relaxation, and cardiovascular stability throughout the procedure.
Pre-anesthetic evaluation starts with bloodwork to assess kidney and liver function, which process anesthetic drugs. Older pets or those with underlying health conditions may require additional testing like chest X-rays or electrocardiograms. During surgery, continuous monitoring tracks heart rate, blood pressure, oxygen levels, and carbon dioxide levels, with trained veterinary technicians adjusting anesthetic depth in real-time.
The choice between inhalant anesthetics (like isoflurane or sevoflurane) and injectable protocols depends on the procedure’s length and complexity. Short procedures might use injectable combinations for quick induction and recovery, while longer surgeries rely on inhalant gases that can be precisely controlled and eliminated rapidly when surgery concludes.
Pain management protocols now begin before surgery starts, with pre-emptive pain medications preventing the establishment of chronic pain pathways. Multi-modal approaches combine different drug classes — opioids, non-steroidal anti-inflammatory drugs, local anesthetics, and newer agents like gabapentin — to control pain through multiple mechanisms while minimizing side effects.
Impact of Surgical Techniques on Recovery
Minimally invasive surgical techniques have revolutionized pet surgery over the past decade, offering significant advantages in recovery time, pain levels, and complication rates. Laparoscopic procedures use small incisions and camera guidance to perform surgeries that traditionally required large abdominal openings. A laparoscopic spay requires two or three half-inch incisions instead of a three-to-four-inch abdominal incision, resulting in dramatically faster healing and reduced post-operative pain.
The difference in recovery becomes apparent within hours of surgery. Pets that undergo traditional open procedures typically require several days of restricted activity and careful incision monitoring. Those that have minimally invasive procedures often return to normal activity within 24-48 hours, though some restrictions still apply to prevent complications.
Surgical approach also affects long-term outcomes. Joint surgeries using arthroscopic techniques preserve more healthy tissue and reduce scar formation compared to open joint exploration. This preservation of normal anatomy often translates to better long-term joint function and reduced arthritis development. However, not all procedures can be performed minimally invasively, and the surgeon’s experience with specific techniques plays a crucial role in determining the best approach for each case.
How to Prepare Your Pet and What Recovery Looks Like

Pre-surgical preparation begins days before the actual procedure with specific instructions designed to optimize surgical safety and outcomes. Most pets require fasting for 8-12 hours before surgery to prevent vomiting and aspiration during anesthesia induction. Water is typically removed 2-4 hours before surgery, though protocols vary based on the pet’s age and health status.
The morning of surgery involves final health assessments, intravenous catheter placement, and pre-anesthetic medications. Many veterinary hospitals begin pain management protocols before surgery starts, providing better pain control throughout the procedure and into recovery. Some pets receive anti-anxiety medications to reduce stress associated with hospitalization and handling.
Recovery timelines vary dramatically based on the procedure’s complexity and invasiveness. Routine spay or neuter surgeries typically involve 7-10 days of activity restriction, with most pets feeling normal within 2-3 days despite needing continued rest. Orthopedic procedures like cruciate ligament repairs require 6-8 weeks of strict activity limitation, with gradual return to normal function over 3-4 months.
Post-operative monitoring focuses on incision healing, pain management, and return to normal function. Owners watch for signs of infection (swelling, discharge, excessive redness), ensure pets aren’t licking or chewing surgical sites, and follow medication schedules precisely. Modern pain management protocols mean most pets should appear comfortable within 24-48 hours of surgery, though some drowsiness from medications is normal.
Activity restrictions protect healing tissues while preventing complications. The temptation to allow early return to normal activity because the pet “seems fine” can result in serious setbacks like incision breakdown, internal bleeding, or implant failure in orthopedic cases. Following discharge instructions precisely, even when pets seem eager to resume normal activities, prevents most post-surgical complications.
Understanding Risks and Managing Complications in Pet Surgery
Every surgical procedure carries inherent risks that veterinarians work systematically to minimize through careful planning, monitoring, and preparation. Anesthetic complications represent the most immediate concern, particularly in older pets or those with underlying health conditions. Modern anesthetic protocols and monitoring equipment have reduced anesthetic mortality rates to less than 0.1% for healthy pets, though risks increase with age and pre-existing disease.
Surgical site infections develop in approximately 2-5% of veterinary surgeries, typically manifesting 3-7 days after the procedure. These infections usually result from bacterial contamination during surgery or post-operative complications like excessive licking or contamination of the incision site. Most surgical site infections respond well to antibiotic therapy when detected early, though severe cases may require surgical revision.
Bleeding complications can occur during or after surgery, ranging from minor oozing that stops on its own to life-threatening hemorrhage requiring emergency intervention. Veterinary surgeons minimize bleeding risks through careful surgical technique, proper instrumentation, and pre-surgical assessment of clotting function in high-risk patients. Post-operative bleeding typically becomes apparent within the first 24-48 hours and may require immediate surgical exploration.
Pain management complications arise when pets don’t respond adequately to standard protocols or experience adverse reactions to pain medications. Some animals metabolize certain drugs differently, requiring dosage adjustments or alternative medications. Signs of inadequate pain control include excessive vocalization, reluctance to move, loss of appetite, or aggressive behavior changes. Conversely, some pets experience sedation or gastrointestinal upset from pain medications, necessitating protocol modifications.
When selecting appropriate pet surgery options, veterinarians carefully weigh potential complications against the benefits of surgical intervention, ensuring owners understand both the expected outcomes and possible risks before proceeding.
The key to managing surgical complications lies in early recognition and prompt intervention. Most complications that develop quickly after surgery can be successfully treated when addressed immediately, emphasizing the importance of following post-operative monitoring instructions and maintaining open communication with the veterinary team throughout the recovery process.
Other Articles You May Find of Interest...
- 10 Questions to Ask Before Buying a Dog or Cat
- Effective Pain and Anxiety Relief: Exploring Gabapentin and Trazodone for Dogs
- Is Trazodone Safe for Cats? Exploring Benefits and Risks
- 2026 Buyer’s Guide: The 9 Best Pet Insurance Plans Ranked by Real Coverage
- The Best 5 Platforms to Find a Dachshund Puppy Safely in 2026
- How Do Bully Sticks Affect Your Dog’s Overall Health? 6 Key Considerations
- Can Dogs Get Norwalk Virus? Understanding the Risks and Symptoms














